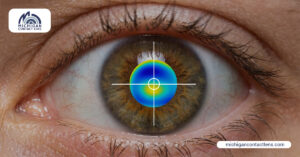
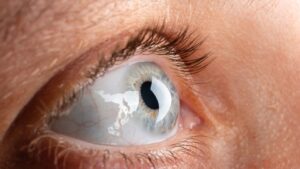
Keratoconus is an eye condition that affects the shape of the cornea, leading to blurred vision that cannot be corrected with glasses. Over time, the cornea thins and bulges outward, resembling a cone shape. It is often diagnosed during the teenage years or early adulthood and progressively worsens as the cornea becomes more irregular.
One common question that arises among people diagnosed with keratoconus is whether the condition is genetic. While the exact cause is still being researched, there is significant evidence to suggest that genetics plays a role in the development of keratoconus.
Frequency of Keratoconus
Keratoconus affects approximately 1 in 2,000 individuals worldwide, though its prevalence may vary based on geographic region, ethnicity, and family history. Studies show that keratoconus is more common in certain populations, particularly in Middle Eastern and South Asian communities.
The condition typically presents in adolescence and progresses slowly. In some cases, it stabilizes in the early twenties, while in others, it can continue to worsen, requiring corneal transplants as a last resort.
Symptoms of Keratoconus
The symptoms of keratoconus develop slowly and often worsen over time. Common early signs include:
- Blurry or distorted vision, particularly at night
- Frequent changes in glasses prescription that no longer correct vision
- Sensitivity to light and glare
- Frequent eye rubbing or irritation due to itchy eyes (common in allergic reactions)
- Double vision or ghosting of images
These symptoms can significantly affect daily activities like driving, reading, or using digital devices.
Causes of Keratoconus
The exact cause of keratoconus remains unknown, but it is believed to be a combination of genetic and environmental factors. Research indicates that certain behaviors, such as eye rubbing (often due to allergies), may exacerbate the condition.
Genetic Factors
- Family History: Individuals with a family history of keratoconus are at a higher risk of developing the condition. Studies show that 5-10% of individuals with keratoconus have a close relative with the condition.
- Genetic Mutations: Several genes have been associated with keratoconus, particularly those involved in the formation and structure of the cornea. Some of these include:
- COL4A3
- COL5A1
- TGFBI (transforming growth factor beta-induced gene)
Research continues to focus on identifying the specific mutations that make individuals more susceptible to the condition.
Environmental Factors
- Eye Rubbing: Frequent or forceful eye rubbing can lead to increased stress on the cornea, which may worsen keratoconus.
- Allergies: Allergic reactions and conditions like hay fever can exacerbate eye rubbing, leading to greater strain on the cornea.
Genetic Inheritance of Keratoconus
Keratoconus tends to run in families, indicating a genetic link to the condition. In many cases, keratoconus follows an autosomal dominant inheritance pattern, which means that inheriting one copy of the mutated gene from either parent is enough to cause the disease.
However, genetic inheritance is complex, and keratoconus can also occur in individuals without a family history, suggesting that environmental factors can also play a significant role.
Inheritance Patterns
- Autosomal Dominant: In families with keratoconus, the condition often follows an autosomal dominant pattern, meaning one parent with the condition has a 50% chance of passing it on to their child.
- Autosomal Recessive: Some cases of keratoconus may follow an autosomal recessive inheritance pattern, where two copies of the mutated gene (one from each parent) are required for the condition to develop.
Why Early Diagnosis Matters
Early diagnosis of keratoconus is critical to slowing its progression and preventing severe visual impairment. Since keratoconus is hereditary, individuals with a family history of the condition should be vigilant for symptoms, especially during adolescence or early adulthood when the disease typically begins.
Early intervention can help preserve vision and may prevent the need for corneal transplants. Regular eye exams are essential for detecting the condition at an early stage, even before significant vision changes occur.
Treatment Options for Keratoconus
There are several treatment options available for individuals with keratoconus, ranging from non-surgical solutions to surgical interventions. The treatment plan depends on the severity of the condition and the age of the patient.
- Eyeglasses and Soft Contact Lenses: In the early stages of keratoconus, glasses or soft contact lenses may be sufficient to correct vision. However, as the condition progresses, they may no longer provide clear vision.
- Rigid Gas-Permeable Contact Lenses: These lenses are often used in moderate to advanced cases of keratoconus. They help provide a smoother surface for light to enter the eye, improving vision.
- Scleral Lenses: Scleral lenses are the most effective contact lenses for keratoconus. They vault over the cornea, creating a stable surface for better vision and comfort. They also help reduce the risk of corneal scarring.
- Corneal Cross-Linking (CXL): Corneal cross-linking is a minimally invasive procedure that helps strengthen the cornea and slow the progression of keratoconus, especially in younger patients.
- Corneal Transplant: In severe cases of keratoconus, when other treatments do not provide adequate vision correction, a corneal transplant may be required to restore vision.
What Are the Genetic Tests for Keratoconus?
Currently, genetic testing for keratoconus is not routinely performed for diagnosis but may be used for individuals with a strong family history of the condition. Genetic counselling can help assess the risk of passing keratoconus to offspring, especially in families with multiple affected members.
There are ongoing studies to identify the specific genetic markers associated with keratoconus, which could lead to earlier diagnosis and more targeted treatments in the future.
Conclusion
While keratoconus is not entirely understood, research has confirmed that genetics plays a key role in the development of this eye condition. If you have a family history of keratoconus, it’s important to be aware of the early symptoms and seek treatment if needed.
Early intervention with treatments like scleral lenses, corneal cross-linking, and regular eye exams can help manage and slow down the progression of keratoconus, improving vision and quality of life.
If you suspect you have keratoconus, or if it runs in your family, consult with an eye care professional for early detection and guidance on the best treatment options.
Frequently Asked Questions
Is keratoconus a genetic condition?
Yes, keratoconus is hereditary in many cases. Studies show that individuals with a family history of keratoconus are at a higher risk of developing the condition. In fact, about 5-10% of keratoconus patients have a close relative who also has it.
Can I get keratoconus if no one in my family has it?
Yes, keratoconus can occur sporadically in individuals without a family history. However, the risk increases if there is a genetic predisposition in the family. Environmental factors, such as eye rubbing or allergies, may also contribute to the development of keratoconus.
Can keratoconus be inherited from one parent?
Yes, keratoconus often follows an autosomal dominant inheritance pattern, meaning if one parent has the condition, there is a 50% chance that it can be passed on to their child. However, keratoconus may not always develop even if the gene is inherited.
How likely is it for children to get keratoconus if one parent has it?
If one parent has keratoconus, their child has a 1 in 10 chance of developing it. However, the risk increases significantly if both parents have the condition.
Can keratoconus skip generations?
Yes, keratoconus can skip generations. A person may inherit the genetic mutation but not develop the disease, only for it to appear in the next generation due to environmental or other triggering factors.
Can keratoconus be prevented with genetic testing?
Currently, genetic testing is not a routine procedure for preventing keratoconus, but it can help identify individuals at higher risk, especially those with a family history. Early genetic counseling can help families make informed decisions about the condition.