Many patients with astigmatism achieve clear vision with glasses or soft contact lenses. However, patients with high astigmatism, irregular corneas, or keratoconus often need a more advanced solution. Scleral lenses are designed to provide clear and more comfortable vision in these situations.
Many patients use toric soft contact lenses to manage regular astigmatism in the early stages. These lenses help stabilize vision by staying aligned on the eye during wear. For more complex or unstable cases, scleral lenses often become the better solution.
Challenges of Astigmatism and Keratoconus
When astigmatism occurs in conjunction with keratoconus, it adds a layer of complexity to vision correction. The irregular shape of the cornea in keratoconus exacerbates the astigmatism, making it difficult to achieve clear and sharp vision.
In order to effectively manage the astigmatism associated with keratoconus, specialized contact lenses are often prescribed. These lenses are designed to conform to the irregular corneal shape, providing improved visual acuity and comfort.
To learn more about other treatment options and the role of scleral lenses in addressing keratoconus, continue reading our article on scleral lenses for keratoconus.
What Makes Scleral Lenses the Best Hard Lens Option for Astigmatism?
When it comes to managing keratoconus and astigmatism, hard contact lenses have long been a popular choice. Among these, traditional rigid gas permeable (RGP) lenses have been widely used to correct vision and improve the visual clarity of individuals with these conditions.
Traditional Rigid Gas Permeable (RGP) Lenses
RGP lenses are made from firm oxygen-permeable materials that help maintain corneal health and improve vision quality. They often work well for patients with keratoconus and irregular astigmatism. Patients may need a short adjustment period before the lenses feel fully comfortable
Limitations of RGP Lenses for Astigmatism
- GP lenses may not fit well on highly irregular corneas caused by advanced keratoconus.
- Some patients still experience blurry vision, ghosting, or halos around lights while wearing them.
- The rigid design can feel uncomfortable, especially during the adjustment period.
- RGP lenses may move on the eye more often during blinking or physical activity.
- Patients with severe astigmatism may need a more stable option like scleral lenses for clearer vision.
- Regular follow up visits are important to monitor lens fit, comfort, and overall eye health
How Scleral Lenses Work for Astigmatism
Traditional contact lenses may not provide the clarity or comfort needed for astigmatism in keratoconus. Scleral lenses offer a better solution by improving vision and comfort. These lenses are designed to help individuals with astigmatism in keratoconus see more clearly and feel more comfortable.
Call us or book an appointment
What are Scleral Lenses?
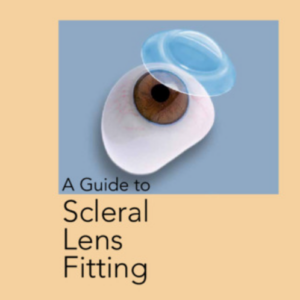
Scleral lenses are a type of hard contact lens that are larger in diameter compared to traditional contact lenses. They are designed to vault over the cornea and rest on the white part of the eye, known as the sclera. These lenses create a tear-filled space between the lens and the cornea, providing a smooth optical surface that helps to correct vision irregularities caused by keratoconus and astigmatism.
Scleral lenses are made from a highly breathable material that allows oxygen to reach the cornea, ensuring long-term eye health. Due to their larger size, they are more stable on the eye and less likely to dislodge during blinking, providing a more comfortable and secure fit.
How Scleral Lenses Help with Astigmatism in Keratoconus
In individuals with both keratoconus and astigmatism, the cornea becomes distorted and irregularly shaped. This irregularity can cause light to scatter and result in blurry or distorted vision. Scleral lenses are uniquely suited to address this issue by correcting the astigmatism and providing a smooth, uniform refractive surface.
The design of scleral lenses allows them to mask the irregularities of the cornea, effectively refracting light and compensating for the astigmatism. By creating a tear-filled reservoir, these lenses provide a stable and consistent optical surface that improves visual acuity and reduces aberrations caused by keratoconus.
Moreover, scleral lenses can also help with other vision-related challenges associated with keratoconus, such as increased sensitivity to light and glare. The larger size of scleral lenses provides a protective barrier, shielding the cornea from environmental irritants and reducing dryness. For more information on how scleral lenses can benefit individuals with keratoconus, check out our article on the benefits of scleral lenses.
By opting for scleral lenses, individuals with astigmatism in keratoconus can achieve improved vision and enhanced comfort throughout the day. However, it’s important to note that the fitting process for scleral lenses is more complex than traditional contact lenses. It involves a thorough assessment of the eye’s shape and measurements to ensure a proper fit. To learn more about the scleral lens fitting process, refer to our article on the scleral lens fitting process.
Scleral lenses provide an advanced and effective solution for individuals with astigmatism in keratoconus, offering improved vision correction, enhanced comfort, and protection for the eyes. If you are considering scleral lenses, consult with a qualified eye care professional who specializes in fitting these lenses to determine if they are the right option for you.
Benefits of Scleral Lenses for Astigmatism
When it comes to managing astigmatism in keratoconus, scleral lenses have emerged as a popular and effective solution. These specialized contact lenses offer several benefits that can significantly improve the vision and overall comfort of individuals with this condition.
Improved Vision Correction
One of the key advantages of scleral lenses for astigmatism is their ability to provide superior vision correction. Due to the irregular shape of the cornea in keratoconus, traditional contact lenses may not adequately correct astigmatism, leading to distorted and blurry vision. However, scleral lenses are designed to vault over the cornea, creating a smooth and even surface for light to pass through. This results in clearer and sharper vision, helping individuals with astigmatism in keratoconus to see more clearly.
Enhanced Comfort and Fit
Scleral lenses are known for their comfortable and secure fit. Unlike traditional rigid gas permeable (RGP) lenses, which can sometimes cause discomfort and irritation, scleral lenses rest on the sclera (the white part of the eye) without touching the cornea. This unique design provides a cushion of fluid between the lens and the eye, offering improved comfort throughout the day. The larger size of scleral lenses also helps to stabilize the lenses on the eye, reducing the chances of lens movement and dislocation.
To ensure optimal comfort and fit, it is crucial to undergo a thorough scleral lens fitting process. This involves taking precise measurements and customizing the lenses to fit the unique contours of the individual’s eyes. The fitting process may involve trial lenses and adjustments to achieve the best possible fit for maximum comfort and vision correction. For more information on the fitting process, refer to our article on the scleral lens fitting process.
Protection and Moisture for the Eyes
Another significant benefit of scleral lenses is their ability to provide protection and moisture to the eyes. The space between the back surface of the lens and the cornea acts as a reservoir for a saline solution, which keeps the cornea hydrated throughout the day. This is especially beneficial for individuals with dry eyes or those who experience discomfort with traditional contact lenses. Scleral lenses create a protective barrier that shields the cornea from external irritants, such as dust and debris, further enhancing the comfort and health of the eyes. To learn more about how scleral lenses can benefit individuals with dry eyes, check out our article on scleral lenses for dry eyes.
In summary, scleral lenses offer several advantages for individuals with astigmatism in keratoconus. These lenses provide improved vision correction, enhanced comfort and fit, and protection and moisture for the eyes. If you are considering scleral lenses as a treatment option for your astigmatism in keratoconus, consult with an eye care professional who specializes in fitting these lenses. They can guide you through the process and help determine if scleral lenses are the right choice for your unique needs.
Considerations for Scleral Lens Wearers
When considering scleral lenses as a treatment option for astigmatism in keratoconus, there are several important factors to keep in mind. These include the fitting process and customization, maintenance and care, as well as potential risks and complications.
Fitting Process and Customization
The fitting process for scleral lenses involves a series of steps to ensure a proper fit and optimal vision correction. It begins with a comprehensive eye examination conducted by an eye care professional specializing in contact lenses for keratoconus. During this examination, detailed measurements of the cornea are taken to create custom-made lenses that suit the unique needs of each individual.
The customization of scleral lenses allows for precise correction of astigmatism in keratoconus. The lenses are designed to vault over the irregular cornea, creating a smooth optical surface that enhances visual clarity. The fitting process may require multiple visits to fine-tune the fit and ensure optimal comfort and vision. For a detailed overview of the scleral lens fitting process, refer to our article on the scleral lens fitting process.
Maintenance and Care for Scleral Lenses
Proper maintenance and care are essential for the longevity and effectiveness of scleral lenses. The following guidelines should be followed to ensure the lenses remain clean and safe for use:
- Cleaning
Scleral lenses should be cleaned daily using a recommended cleaning solution. This helps remove debris, protein deposits, and bacteria that may accumulate on the lens surface. - Storage
After cleaning, the lenses should be stored in a sterile saline solution or a disinfecting solution recommended by the eye care professional. - Hygiene
Clean hands are essential when handling scleral lenses. Thoroughly wash and dry your hands before inserting or removing the lenses to minimize the risk of contamination. - Follow-up Visits
Regular follow-up visits with your eye care professional are crucial to monitor the health of your eyes and the condition of the lenses. These visits also provide an opportunity to address any concerns or discomfort you may be experiencing.
For more information on maintaining healthy eyes while wearing scleral lenses, consult with your eye care professional or refer to our article on scleral lenses for dry eyes.
Potential Risks and Complications of Scleral Lenses
While scleral lenses can provide significant benefits for astigmatism in keratoconus, it is important to be aware of potential risks and complications. These may include:
- Discomfort
Some individuals may experience initial discomfort or a foreign body sensation when wearing scleral lenses. This can often be managed by adjusting the fit or using lubricating eye drops as recommended by the eye care professional. - Dryness
Dryness may occur due to reduced oxygen permeability. However, scleral lenses are designed to trap a layer of tears between the lens and the cornea, providing moisture and protection. Eye drops or artificial tears may be used to alleviate any dryness symptoms. - Infection
Although rare, the risk of infection exists with any type of contact lens wear. Proper hygiene, regular follow-up visits, and adherence to the recommended cleaning and storage protocols are crucial in minimizing this risk.
If you experience persistent discomfort, redness, or any unusual symptoms while wearing scleral lenses, it is important to consult your eye care professional immediately. They will be able to address any concerns and provide appropriate guidance.
By considering the fitting process, maintenance, and care, as well as potential risks and complications, scleral lens wearers can make informed decisions and maximize the benefits of this treatment option for astigmatism in keratoconus. Remember to follow the recommendations of your eye care professional and attend regular follow-up visits to ensure the best outcomes for your vision and eye health.
Scleral Lenses vs. Toric Soft Lenses for Astigmatism
Many patients use toric soft contact lenses to manage regular astigmatism in the early stages. These lenses help stabilize vision by staying aligned on the eye during wear. For more complex or unstable cases, scleral lenses often become the better solution.
| Feature | Toric Soft Lenses | Scleral Lenses |
|---|---|---|
| Works for irregular astigmatism | No — relies on a regular corneal shape | Yes — vaults over the entire cornea |
| Stable vision throughout the day | Can rotate and fluctuate | Very stable — rests on the sclera |
| High astigmatism correction (−3.00 D+) | Limited range; often suboptimal | Custom-made for any prescription |
| Suitable after LASIK/corneal surgery | Often ineffective on altered corneas | Designed for post-surgical corneas |
| Comfort with dry eyes | Can worsen dryness | Tear reservoir keeps cornea hydrated |
| Fitting complexity | Simple — off-the-shelf sizes | Custom fitting required — multiple visits |
| Upfront cost | Lower | Higher — but often covered in part by insurance |
Scleral lenses often perform better than toric lenses for patients with high astigmatism or irregular corneal conditions. They provide more stable vision and improved comfort throughout the day for many patients. If your toric lenses rotate often or leave your vision blurry, scleral lenses may be a better option.
Scleral Lens Specialist in Michigan
Dr. Shira Kresch provides scleral lens exams for patients across Michigan, including Metro Detroit, Troy, and Birmingham. Patients with keratoconus and astigmatism often need custom scleral lens fitting to achieve clear vision and long term comfort.
Frequently Asked Questions
Can scleral lenses correct astigmatism?
Yes, scleral lenses can correct astigmatism, including irregular astigmatism caused by keratoconus or corneal damage. These lenses create a smooth optical surface over the cornea, which allows light to focus properly and improves vision when glasses or soft contact lenses do not work well.
Are scleral lenses good for keratoconus?
Scleral lenses are one of the most effective treatments for keratoconus. They rest on the white part of the eye and cover the irregular cornea, helping patients achieve clearer vision and better comfort. Many people with keratoconus see better with scleral lenses than with glasses or regular contact lenses.
Why are scleral lenses better for irregular astigmatism?
Irregular astigmatism causes uneven focusing of light, which makes vision blurry or distorted. Scleral lenses help by covering the irregular shape of the cornea and creating a smooth surface for vision. This allows patients to see more clearly and comfortably compared to standard contact lenses.
Do scleral lenses help blurred vision?
Yes, scleral lenses often help blurred vision caused by keratoconus, astigmatism, dry eye, or corneal scars. Because the lens vaults over the cornea and holds a layer of fluid, it provides more stable and sharper vision than regular contact lenses.
Can keratoconus cause astigmatism?
Yes, keratoconus often causes irregular astigmatism because the cornea becomes uneven and cone shaped. This makes it difficult for light to focus correctly. Scleral lenses are commonly used for keratoconus because they can improve vision by covering the irregular cornea.