Still Seeing Halos and Glare Even With Scleral Lenses?You finally got fitted for scleral lenses. Your vision is better. But at night, there are still halos around headlights. Lights streak. Driving feels unsafe. Objects ghost or double. If this sounds familiar, you are not imagining it, and it is not a fitting problem.
This is what’s called residual higher-order aberrations (HOAs), complex optical distortions that even the best standard scleral lens cannot correct. The good news: wavefront guided scleral lenses are specifically engineered to fix exactly this.
What Are Higher-Order Aberrations (HOAs)?
Most people are familiar with lower-order aberrations: nearsightedness, farsightedness, and regular astigmatism. These are corrected by standard glasses and contacts. Higher-order aberrations are a different category entirely, complex distortions inside the eye’s optical system that cause:
Halos
Glowing rings that form around light sources like streetlights, traffic signals, or oncoming headlights at night. They occur when light scatters around the irregularly shaped cornea instead of focusing cleanly on the retina. For keratoconus patients or those with post-surgical corneas, halos can be large enough to obscure the light source itself, making nighttime navigation genuinely dangerous.
Glare
An overwhelming wash of brightness that floods your vision when exposed to headlights, bright lamps, or reflective surfaces. Unlike halos, glare spreads diffusely across your entire visual field rather than forming a defined ring, making it feel like looking directly into a bright light even when you are not. Many patients describe it as a blinding veil that wipes out contrast and fine detail in the surrounding scene.
Starbursts
Sharp spikes or rays of light that radiate outward from a point source, making a single streetlight look like a firework or exploding star. They are caused by specific HOAs called coma and trefoil, which pull light into asymmetric patterns across the retina. Patients with keratoconus often experience starbursts in a directional pattern — the spikes tend to shoot consistently in one direction based on the cone’s position on the cornea.
Ghosting / Double Vision
A secondary faint copy of an image that appears offset from the real one, as if the world has a shadow version of itself slightly displaced to one side. This happens because different zones of the irregular cornea bend light at slightly different angles, creating two overlapping focal points instead of one clean image. Reading, watching screens, and recognizing faces all become noticeably harder, and the effect typically worsens in lower light when the pupil dilates and exposes more of the aberrated cornea.
Smearing
A dragging, streaky distortion where edges of objects appear to bleed or smudge in one direction, similar to a photograph taken with a sideways camera shake. It is caused by coma, a higher-order aberration that pulls the focal point of light into a comet-like tail rather than a sharp point. Text on signs, display boards, and phone screens can become nearly unreadable, as letters appear to melt into each other rather than sitting cleanly on the line.
Low-Contrast Fatigue
A less obvious but deeply exhausting symptom where the visual system struggles to distinguish objects from their backgrounds in dim, overcast, or foggy conditions. While a person’s measured Snellen acuity might read 20/20 in a bright clinical setting, real-world performance degrades significantly in low-contrast environments like rainy evenings, foggy mornings, or dimly lit rooms. Over time this forces the brain to work harder to interpret every visual scene, leading to headaches, eye strain, and a general sense of visual tiredness by the end of the day.
Standard scleral lenses create a smooth refracting surface that corrects corneal irregularities. But they do not, and cannot, neutralize internal aberrations from the back of the cornea or the lens. This is why some patients with a perfectly fitted scleral lens still report poor visual quality, especially at night.
Types of Higher-Order Aberrations (HOAs)
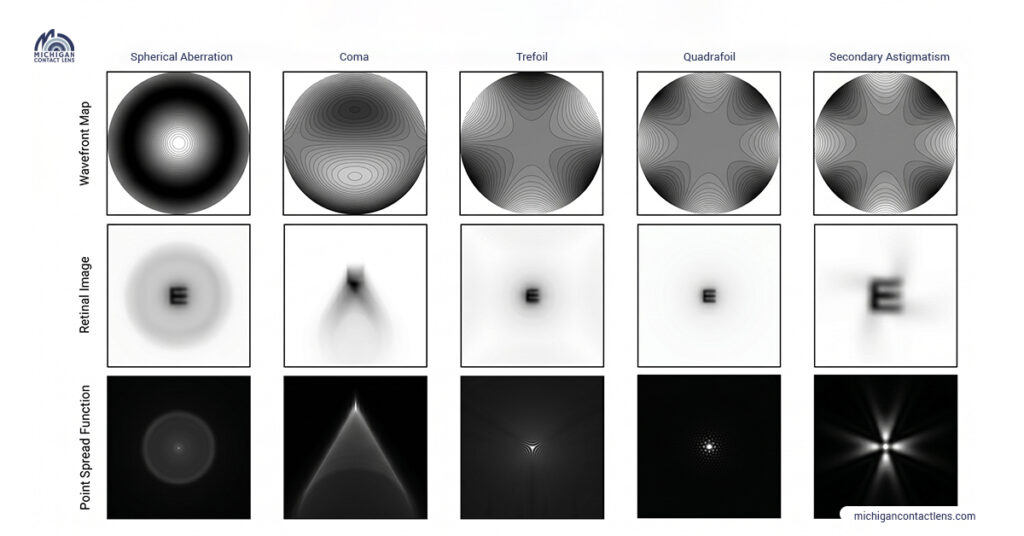
Higher-order aberrations are not a single problem, they are a family of distinct optical distortions, each caused by a different irregularity in the eye’s optical system. Understanding which specific aberrations you have is exactly what wavefront aberrometry measures, and what your custom lens is built to correct.
Coma
Coma is one of the most common HOAs in keratoconus patients. It occurs when light rays passing through different parts of the cornea focus at slightly different points, creating a comet-like smear or tail stretching in one direction from every light source. Patients with coma often describe seeing streaks or smearing radiating consistently in the same direction, not randoml, because the distortion follows the shape and position of their corneal cone. It is the primary cause of the ghosting and smearing that makes reading and screen use so difficult.
Trefoil
Trefoil produces a three-pointed starburst pattern around light sources, making a single streetlight or headlight appear to have three distinct spikes radiating outward in a triangular formation. It is caused by a three-way asymmetry in the corneal surface and is frequently present alongside coma in keratoconus eyes. Many patients describe trefoil as making every light source look like a spinning star or a three-armed flare, which becomes especially disorienting when driving at night with multiple light sources in view simultaneously.
Spherical Aberration
Spherical aberration occurs when light passing through the center of the cornea and light passing through the edges focus at different distances, creating a soft, unfocused halo or blur around objects and light sources. Unlike coma and trefoil which produce directional distortions, spherical aberration is symmetrical, the halo or glow appears evenly around the entire light source in all directions. It worsens significantly at night when the pupil dilates and exposes more of the peripheral cornea, which is precisely where the focusing mismatch is greatest.
Secondary Astigmatism
Secondary astigmatism is a more complex version of regular astigmatism that cannot be corrected by standard cylindrical lenses in glasses or soft contacts. It arises from irregular corneal curvature that varies across different zones of the eye rather than following a simple two-axis pattern. Patients experience a layered blur where vision appears distorted in ways that glasses simply cannot touch, no matter how carefully the prescription is refined, a common source of frustration for keratoconus patients who have been told their glasses prescription is “as good as it can get.”
Quadrafoil
Quadrafoil is similar to trefoil but produces a four-pointed starburst pattern around light sources rather than three. It is less common than coma and trefoil but still measurable by aberrometry and correctable with wavefront-guided lenses. Patients with quadrafoil often describe seeing cross-shaped or four-armed spikes around bright lights, particularly oncoming headlights at night, which can make highway driving feel genuinely unsafe.
What Are Wavefront-Guided Scleral Lenses?
Wavefront-guided scleral lenses use the same technology originally developed for space telescopes to capture sharper images of distant stars. Applied to the eye, wavefront aberrometry precisely measures every distortion in your optical system, not just the cornea, but the entire visual pathway.
The result is a custom-ground lens that uses destructive interference to cancel out your specific HOAs — the same principle as noise-canceling headphones. Your unique distortions are measured, mapped, and an equal-and-opposite optical correction is built directly into the lens surface.
How are Wavefront Guided Scleral Lenses Fitted?

Wavefront-guided scleral lenses are not simply ordere,how are wavefront guided scleral lenses fitted they are built around your individual optics. Here’s what the process looks like:
Standard scleral lens fitting
First, a traditional scleral lens is fitted and optimized for comfort, vault, and basic vision correction. The lens must be stable on the eye before wavefront measurements can be taken.
Aberrometry measurement.
Using a device such as the OVITZ xwave aberrometer, your doctor measures your residual HOAs while you are wearing the fitted lens. This captures exactly what distortions remain after the standard lens has done its work.
Wavefront map creation
Your distortions are broken down into individual Zernike coefficients — mathematical representations of specific aberration types like coma, trefoil, and spherical aberration.
Custom lens manufacturing.
A freeform optical pattern is ground into the front surface of your scleral lens, targeting your exact aberrations.
Lens stabilization
Because the wavefront correction is orientation-specific, the lens must not rotate. Toric haptics or quadrant-specific designs are used to lock the lens in place on your eye.
What Does the Clinical Research Say?
This is not experimental technology. The evidence is strong.
Research led by Dr. John Gelles, OD, published in Eye & Contact Lens, showed
- 56% reduction in higher-order aberrations compared to traditional scleral lenses
- 71% of patients improved by 1 or more lines of visual acuity
- 94% of patients preferred their vision with wavefront-guided lenses over traditional scleral lenses
A separate case series using Zenlens Chroma wavefront-guided lenses found an average HOA reduction of 73.5% across all eyes, with patients reporting significant improvement in subjective vision quality.
Who Is a Good Candidate?
Wavefront-guided scleral lenses work best for patients who:
- Are already successfully wearing standard scleral lenses with good comfort and wear time, but are still experiencing visual distortions
- Have 1–2 specific aberration types dominating their visual complaints (coma, trefoil, spherical aberration)
- Have rotationally stable lens fits — the wavefront correction only works if the lens stays put
- Suffer from keratoconus, post-LASIK complications, corneal scarring, or post-transplant irregular corneas
Conditions commonly treated:
- Keratoconus (the most common indication)
- Post-LASIK or post-RK complications with persistent glare and halos
- Corneal trauma or scarring with residual aberrations
- Post-penetrating keratoplasty (corneal transplant) with irregular astigmatism
- Corneal ectasia after refractive surgery
Who may benefit less: Patients with active cataracts (surgery is often the more direct solution), corneal scars directly in the optical zone, or lenses that rotate frequently on the eye.
Why Night Vision Specifically Improves
Night driving is where most patients notice the biggest improvement, and there’s a clear optical reason.
At night, your pupil dilates. This exposes more of the peripheral cornea, the most aberrated part in conditions like keratoconus. A larger pupil means more HOA-affected light enters the eye, which is why glare, halos, and starbursts get dramatically worse after dark.
Wavefront-guided lenses correct aberrations across a larger optical zone, compensating for pupil dilation. Many patients describe the change as going from “every headlight looks like an explosion“ to seeing clean, distinct lights.
Neuroadaptation: What to Expect During Adjustment
Some long-term keratoconus patients experience an interesting adjustment period. After years of seeing distorted images, the brain has adapted to that distorted input as “normal.” When wavefront-guided lenses suddenly deliver high-definition vision, it can feel disorienting, almost too sharp at first.
This is called neuroadaptation. It is temporary. Most patients fully adjust within a few weeks and describe the final result as the clearest vision they have ever experienced.
How Much Do Wavefront-Guided Scleral Lenses Cost?
Wavefront-guided scleral lenses are premium medical devices. Costs are higher than standard scleral lenses due to:
- Advanced aberrometry diagnostic equipment
- Custom freeform lens manufacturing
- Wavefront software licensing fees
- Additional fitting appointments required
While pricing varies by practice and the complexity of your prescription, most patients consider the investment worthwhile given the improvement in daily functioning, night driving safety, and quality of life. Insurance coverage varies, contact our office to discuss your specific situation.
Are Wavefront-Guided Scleral Lenses Available in Michigan?
If you are in the Metro Detroit area — Troy, Birmingham, Oakland County, or surrounding communities, and are struggling with glare, halos, or visual distortion despite wearing scleral lenses, our practice specializes in advanced scleral lens fitting including wavefront-guided options.
Schedule a scleral lens consultation →
Frequently Asked Question
Can I get wavefront-guided lenses if I’ve never worn scleral lenses before?
Not immediately. You need to first be successfully fitted with a standard scleral lens. The wavefront measurements are taken over the fitted base lens, so a stable standard fit is the required foundation.
Do wavefront-guided scleral lenses guarantee 20/20 vision?
Not always, especially in advanced keratoconus or significant corneal scarring. However, most patients see significant improvement in visual quality, contrast sensitivity, and night vision even when acuity numbers don’t change dramatically.
How long do the lenses last?
Typically 1–2 years with proper care, similar to standard scleral lenses. The wavefront correction is permanent in the lens material.
Will my lenses need to be remade if my prescription changes?
Yes. If your cornea changes significantly — particularly with progressing keratoconus — the wavefront map may need to be remeasured and new lenses ordered.
Can I wear these with dry eyes?
Yes. Because wavefront-guided lenses still have the scleral lens architecture (vaulting the cornea with a fluid reservoir), they offer the same dry eye relief as standard scleral lenses.